Health Benefits Solutions Representative - Chandler, AZ
Bank of America - Chandler, AZ
Health Benefits Solutions Representative - Chandler, AZ

Oops! This job has expired, but don’t worry.
Explore other exciting job listings and take the next step in your career journey!
115
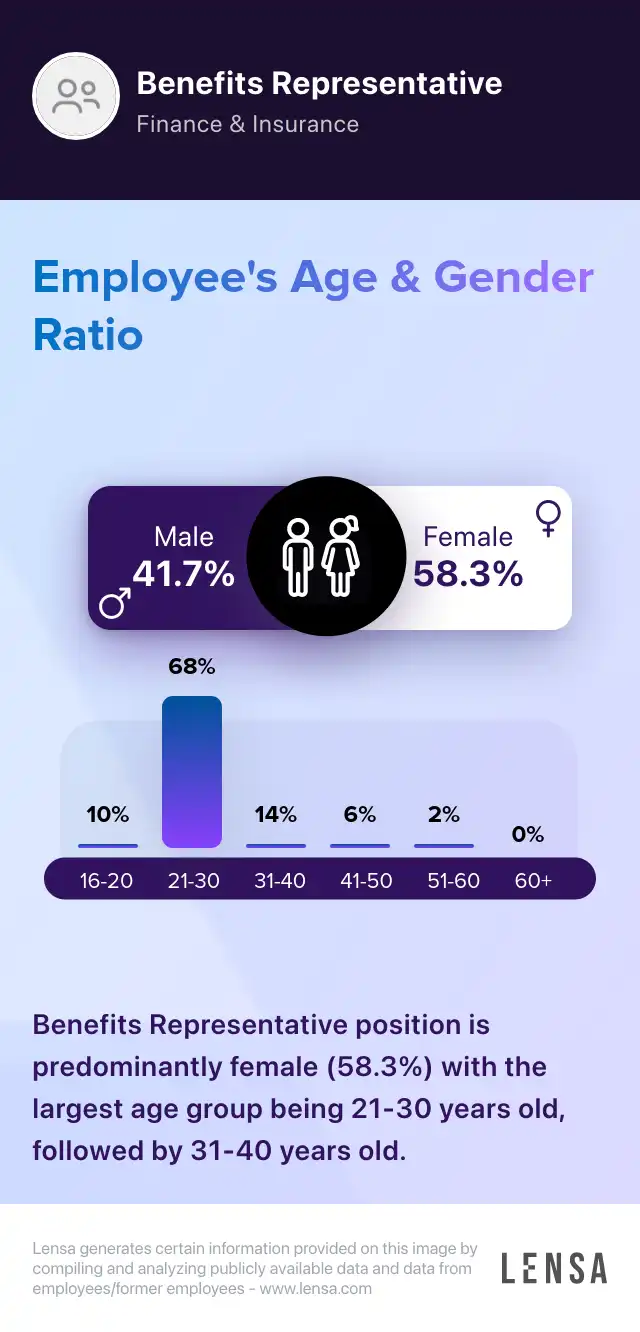
Benefits Representative
jobs978
jobs in
Chandler, AZ
68
jobs at
Bank of America
Job
Company
Description
Salary
Skills
Benefits
Job Description
Health Benefits Solutions Representative - Chandler, AZ
Chandler, Arizona
Job Description:
Associate is accountable for providing quality customer service support within their business unit for some Advisory, FAC and MLD clients requesting retail, retirement and brokerage account products/ service features through inbound calls or emails utilizing professional oral, written and problem solving skills. Accountabilities include but are not limited to providing account balances and activity, deposit rates, checking information, internal systems assistance, explaining and processing transactions. Recommend some previous experience in the customer service field but not required. Elevated service issues handled by experienced associates or above.
Multiple shifts may be available
Role Overview
As a Health Benefits Solutions Representative, you will be working in an inbound contact center taking over 50 calls per day and/or chatting online with clients asking questions or inquiring about their Heath Savings Account (HSA) or Flexible Spending Account (FSA).
What you’ll do
As a Health Benefits Solutions Representative you will be responsible for the following via phone and/or online chat:
-
Providing every client with clear, complete and accurate responses to their questions and inquiries, while updating the system with notes on each client interaction
-
Guiding clients step by step through how to execute various transactions on their accounts (i.e. filing a claims, ordering debit cards, password resets, suspend lost/stolen cards locating statement or tax documents etc.)
-
Ensure client privacy is protected by authenticating each call and not answering questions or providing information to unauthorized users
-
Effectively managing risk by fully adhering to processes/policies/procedures and proactively identifying and escalating potential risks
-
Navigating through multiple applications and tools to understand processes/policy/procedures and research and resolve issues with client accounts
-
May also be trained on the basics of 401(k) retirement accounts to assist as needed with call volume across the Retirement and Health Benefits Solution Contact Center space
Required Skills & Experience (minimum qualifications)
-
Minimum one year experience verbally delivering complex information clearly, concisely and with empathy, while quickly establishing trust and exuding positivity and confidence
-
Must possess the skills to navigate between multiple screens and keep the client/recipient fully engaged, while quickly and accurately typing relevant notes and information
-
Proven ability to professionally and tactfully handle confrontational and/or stressful interactions
-
Demonstrated written communication skills with the ability to type error-free, clear, descriptive and succinct instructions and responses, while being proficient on the keyboard
-
Proven experience with effectively reviewing documentation/files, quickly identifying errors and taking action to resolve the errors
-
Must have experience gathering, absorbing and using facts/information to make effective and timely decisions
-
Demonstrated ability to quickly learn, adapt and become highly efficient on new and/or changing systems, applications, policies and procedures
-
Must be able to succeed in an environment in which you are constantly being held accountable for metrics
Required to work from the primary work location listed when not in remote operating stance
-
Initially you may be required to work from home and/or remotely in this role:
-
Internet Service Provider at home (no public WiFi or Internet)(high speed internet access and a secure or password-protected internet connection)
Desired Skills & Experience
-
Experience working in a client focus environment
-
Knowledge of Heath Savings Account (HSA) or Flexible Spending Account (FSA)
Job Band:
H7
Shift:
1st shift (United States of America)
Hours Per Week:
40
Weekly Schedule:
Referral Bonus Amount:
0
Job Description:
Associate is accountable for providing quality customer service support within their business unit for some Advisory, FAC and MLD clients requesting retail, retirement and brokerage account products/ service features through inbound calls or emails utilizing professional oral, written and problem solving skills. Accountabilities include but are not limited to providing account balances and activity, deposit rates, checking information, internal systems assistance, explaining and processing transactions. Recommend some previous experience in the customer service field but not required. Elevated service issues handled by experienced associates or above.
Multiple shifts may be available
Role Overview
As a Health Benefits Solutions Representative, you will be working in an inbound contact center taking over 50 calls per day and/or chatting online with clients asking questions or inquiring about their Heath Savings Account (HSA) or Flexible Spending Account (FSA).
What you’ll do
As a Health Benefits Solutions Representative you will be responsible for the following via phone and/or online chat:
-
Providing every client with clear, complete and accurate responses to their questions and inquiries, while updating the system with notes on each client interaction
-
Guiding clients step by step through how to execute various transactions on their accounts (i.e. filing a claims, ordering debit cards, password resets, suspend lost/stolen cards locating statement or tax documents etc.)
-
Ensure client privacy is protected by authenticating each call and not answering questions or providing information to unauthorized users
-
Effectively managing risk by fully adhering to processes/policies/procedures and proactively identifying and escalating potential risks
-
Navigating through multiple applications and tools to understand processes/policy/procedures and research and resolve issues with client accounts
-
May also be trained on the basics of 401(k) retirement accounts to assist as needed with call volume across the Retirement and Health Benefits Solution Contact Center space
Required Skills & Experience (minimum qualifications)
-
Minimum one year experience verbally delivering complex information clearly, concisely and with empathy, while quickly establishing trust and exuding positivity and confidence
-
Must possess the skills to navigate between multiple screens and keep the client/recipient fully engaged, while quickly and accurately typing relevant notes and information
-
Proven ability to professionally and tactfully handle confrontational and/or stressful interactions
-
Demonstrated written communication skills with the ability to type error-free, clear, descriptive and succinct instructions and responses, while being proficient on the keyboard
-
Proven experience with effectively reviewing documentation/files, quickly identifying errors and taking action to resolve the errors
-
Must have experience gathering, absorbing and using facts/information to make effective and timely decisions
-
Demonstrated ability to quickly learn, adapt and become highly efficient on new and/or changing systems, applications, policies and procedures
-
Must be able to succeed in an environment in which you are constantly being held accountable for metrics
Required to work from the primary work location listed when not in remote operating stance
-
Initially you may be required to work from home and/or remotely in this role:
-
Internet Service Provider at home (no public WiFi or Internet)(high speed internet access and a secure or password-protected internet connection)
Desired Skills & Experience
-
Experience working in a client focus environment
-
Knowledge of Heath Savings Account (HSA) or Flexible Spending Account (FSA)
Shift:
1st shift (United States of America)
Hours Per Week:
40
Learn more about this role
Full time
JR-21057710
Band: H7
Manages People: No
Travel: No
Manager:
Talent Acquisition Contact:
Dennis Daniel
Referral Bonus:
0
Bank of America and its affiliates consider for employment and hire qualified candidates without regard to race, religious creed, religion, color, sex, sexual orientation, genetic information, gender, gender identity, gender expression, age, national origin, ancestry, citizenship, protected veteran or disability status or any factor prohibited by law, and as such affirms in policy and practice to support and promote the concept of equal employment opportunity and affirmative action, in accordance with all applicable federal, state, provincial and municipal laws. The company also prohibits discrimination on other bases such as medical condition, marital status or any other factor that is irrelevant to the performance of our teammates.
To view the "EEO is the Law" poster, CLICK HERE (https://www.dol.gov/ofccp/regs/compliance/posters/pdf/eeopost.pdf) .
To view the "EEO is the Law" Supplement, CLICK HERE (https://www.dol.gov/ofccp/regs/compliance/posters/pdf/OFCCP_EEO_Supplement_Final_JRF_QA_508c.pdf) .
Bank of America aims to create a workplace free from the dangers and resulting consequences of illegal and illicit drug use and alcohol abuse. Our Drug-Free Workplace and Alcohol Policy (“Policy”) establishes requirements to prevent the presence or use of illegal or illicit drugs or unauthorized alcohol on Bank of America premises and to provide a safe work environment.
To view Bank of America’s Drug-free workplace and alcohol policy, CLICK HERE .
This job was posted on Thu Nov 11 2021 and expired on Wed Nov 24 2021.
Find out how you match this company


Bank of America
Commercial Banking Companies
Reviews
Summary
Bank of America is one of the world's largest financial institutions, serving individuals, small- and middle-market businesses and large corporations with a full range of banking, investing, asset management and other financial and risk management products and services. The company serves approximately 56 million U.S. consumer and small business relationships. It is among the world's leading wealth management companies and is a global leader in corporate and investment banking and trading. The company strives to help all of its employees reach their full potential, with a culture that promotes mutual trust, shared ownership and accountability as well as diversity and inclusion. Bank of America is seeking to hire individuals with a genuine interest in the business and a passion for serving clients, and places a premium on knowledge in different areas and diverse experience.
How do you stay updated on changes in benefits regulations?
Answer
I regularly attend seminars and workshops, and subscribe to industry newsletters to stay informed on the latest changes in benefits regulations.
Can you describe your experience in handling employee benefit inquiries?
How do you ensure accuracy and confidentiality when handling sensitive employee benefit information?

About the Benefits Representative role
Compensation & Benefits Benefits Representative
We, benefits representatives, create the benefit packages for the employees. We manage the benefits packages. We plan the benefit packages according to job and seniority. We answer the queries about the benefit coverage. Some of us also review the agreements for developing the plan. We organize the benefit materials. We also issue the benefit materials. Some of us also educate the employees about different benefits. We plan the orientations and staff meetings. We oversee every benefit program, such as retirement, disability, and medical benefits. We help employees fix benefit-related problems in a timely way. We ensure that employees are updated about the benefits.
Core tasks:
- conducting the surveys regarding benefit industry
- maintaining log of benefit campaigns
- assisting with the events and recognition plans
115 Benefits Representative jobs in Chandler, AZ

Similar jobs in the area